This article sheds light on the most crucial issue – the health of Somali people. Unfortunately, Somalia is currently performing poorly on most statistics regarding development and global health. One of the most important statistics is the life-span.
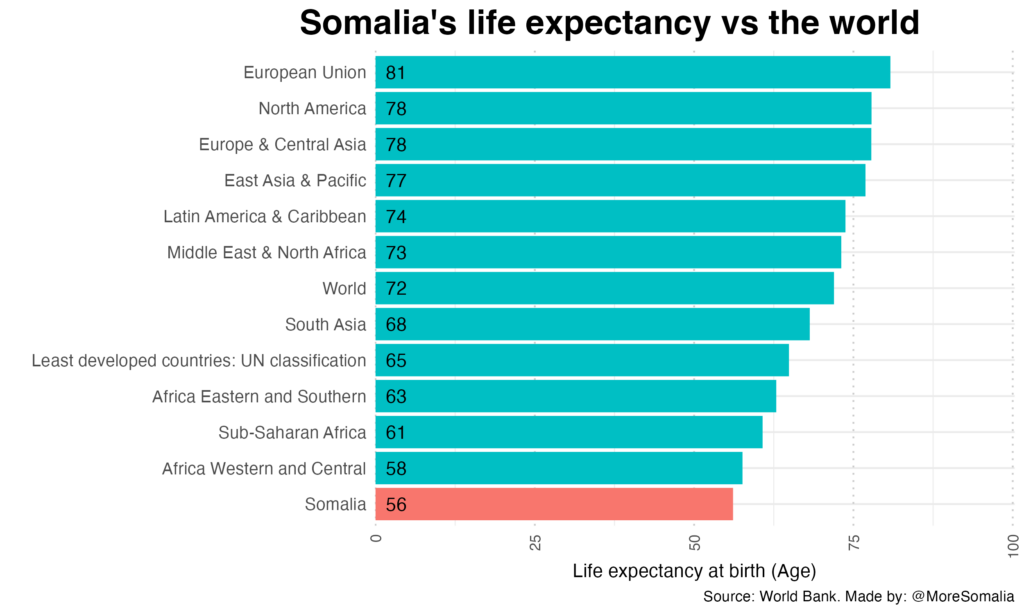
So why is that? What is killing the Somali people?
Well firstly, this is largely caused by three decades of prolonged war and conflicts, which devastated the healthcare infrastructure. When estimating the burden of disease in Somalia (meaning the illnesses that take the greatest toll on the population) infectious diseases stand out. Five of the top 10 causes of death in Somalia are infectious diseases – the most common of which are lower respiratory diseases (e.g. pneumonia) and at second place diarrhoeal diseases (e.g. cholera). The next two causes of death are also related to infectious diseases: At the 3rd place we have “Childhood-cluster diseases” which are various infectious diseases that are easily prevented through childhood vaccine programs, and the 4th most common cause for death is tuberculosis.
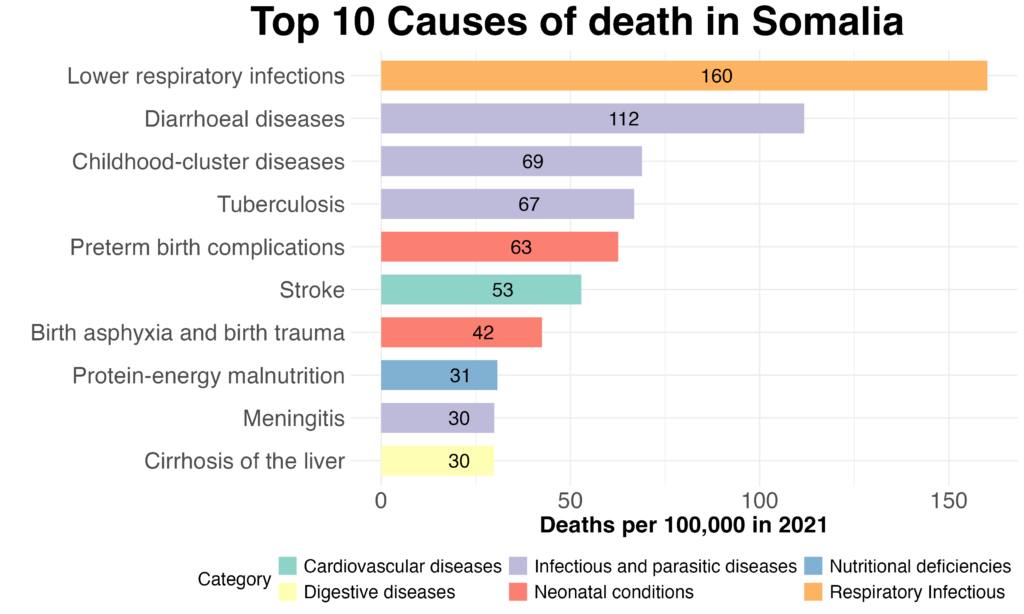
Let’s dive a little more into these common killers. Among the critical infectious diseases three have been selected to explore which provide an overview of Somalia’s public health challenges. Leading the list is cholera, the most well-known of the three.
The fight against infectious diseases in Somalia
Cholera
Unfortunately, cholera continues to claim Somali lives, especially among vulnerable groups. Cholera is an acute diarrheal infection caused by consuming food or water infected with the Vibrio cholerae bacteria. It can cause severe acute watery diarrhea, which can be lethal within hours if not treated. The situation worsens with climate change and Somalia’s harsh weather plays a role in the spread of the disease. Cholera cases usually peak in the Gu rainy season and are worsen during flooding and drought disasters where they lead to contaminated water sources and displaced people, setting the stage for widespread cholera outbreaks. For instance, severe droughts, like the one in 2017, forced people to rely on unsafe water sources, exacerbating the crisis. In 2017 alone, about 78,000 suspected cholera cases were reported, with more than 1,100 deaths (Lubogo et al., 2023). This was particularly devastating, but the harsh truth is that cholera remains endemic in Somalia. As long as water, sanitation, and hygiene (WASH) systems remain weak, outbreaks are expected to occur every year.
Tuberculosis
While cholera grabs headlines, tuberculosis (TB), and particularly its multidrug-resistant form, poses an equally serious threat. TB is endemic to Somalia caused by Mycobacterium tuberculosis. It typically affects the lungs and spreads by droplets from infected people. Somalia is one of the countries with the highest rates of multidrug-resistant tuberculosis (MDR-TB) in the world according to ‘doctors without borders’. What makes this disease dangerous is its airborne nature much like COVID-19, allowing it to spread rapidly within communities. To make matters worse MDR-TB does not respond well to regular antibiotics, and the consequence of this is that Somali patients are left with limited and often costly treatment options, if treatment is even available. So why do these resistant bacteria develop in the first place? Usually due to incomplete or improper treatment, misuse of antibiotics (e.g. not finishing the medicine even if you feel healthy using half), lack of quality medications, and a weak healthcare system.
Sometimes, science has its limits, which is why experts emphasize the need for stricter regulations on antibiotic use. A study found that 13% of reported TB cases in Somalia were multidrug-resistant which is exceptionally high for regional standards (Mohamed et al., 2023).
Treating TB is expensive, and MDR-TB is even more expensive. Somalia’s healthcare budget for TB is insufficient, relying heavily on international donors. In 2021, the total funding for TB in Somalia was $11.1 million, with 100% coming from international sources (Federal gov. of Somalia – Minster of Health & Human Services).
The cost of treating a single MDR-TB patient is estimated to be between $3,500 and $5,900 (Sindani et al. 2013). This financial burden impacts both the government and the individual patients, putting more strains on the scarce resources. The government’s excessive dependency on external funding and rising rates of antibiotic resistance raises questions about the long term sustainability of TB control.
Pneumonia
The third and final disease on the list is pneumonia which is an illness that affects the lungs and a silent killer that devastates families and steals the future from Somali children. While mothers and children are the most vulnerable groups in terms of diseases, pneumonia particularly affects children. It casts the longest shadow over Somali children. In 2018 alone, it accounted for nearly 21% of child deaths and was the leading cause of mortality among children under five. According to UNICEF, pneumonia killed more than 15,165 Somali children under five which is equivalent to over two children every hour (Adawe et al., 2023). While pneumonia takes lives so easily, preventing it is straightforward: vaccination. However a survey released in December 2020 revealed that 60% of Somali children aged 12-23 months had not received any of the four required immunizations (Mohamoud et al., 2024). Without public immunization, preventable diseases will continue to threaten children’s lives.
A path forward
Vaccination as a strategy to reduce infections
The best cure is prevention. While pneumonia is the leading preventable baby killer, it’s not the only one. Childhood-cluster diseases such as ‘whooping cough’, ‘Diphtheria’, ‘Measles’, and ‘Tetanus’ also claim the lives of thousands of young Somali lives. Vaccination coverage for these diseases remains dangerously low in Somalia: The average of coverage for these diseases is at 43%. To effectively protect children, Somalia needs to reach at least 90% coverage. Somalia aims to reduce under-five mortality to 25 per 100,000 by 2030, in line with SDG 3.2. Efforts to reach this goal include introducing PCV and Rotavirus vaccines, expected to save over 35,000 children’s lives annually.
The harsh truth is that childhood diseases are at a minimum in the countries that routinely vaccinate their population. Why is the rate of vaccination so low in Somalia? How can we increase it and save more lives?
Surveillance: Keeping the bacteria in check
After getting an overview of these health challenges, the next step is to explore Somalia’s response. To combat infectious diseases, it is necessary to investigate the pathogens and their effects on the population. The method often used is surveillance which is monitoring health trends to detect patterns of disease transmission. This allows for quicker responses rather than reacting only when outbreaks have already spiraled out of control. The key to controlling these three diseases lies in prevention and early intervention. Since 2023, Somalia has begun implementing a surveillance system called the Integrated Disease Surveillance System, created in 2021. The program has made progress, with 412 hospitals reporting cases weekly – 20 of them are private along with seven laboratories, one national reference lab, and six state laboratories. There are 44 notifiable diseases that these centers must report, allowing authorities to track outbreaks and trends over time. This program is supported by the WHO, and brings great hope in surveillance of diseases.
Somalia appears to be making the right moves in combating infectious diseases, but the question remains: why are the number of cases still so persistently high when on paper the government is doing better?
So, what is actually the problem?
We’ve had meetings with Somali laboratory managers, researchers, politicians, and international technicians over the past 4 months to figure out why the infectious diseases continue to threaten so many lives in Somalia and why it hasn’t been solved.
The numbers don’t fit
From discussions with specialists and those working within the surveillance program, It can be assumed that Somalia’s biggest challenge is lack of funds and proper management. According to multiple sources the lack of funding hinders the ability to hire skilled workers leaving employees underpaid and less motivated to do their duties effectively. Due to the lack of funding an “opportunistic phenomenon” is created in Somalia, where individuals volunteer in labs in the hope of securing a well-funded project in the future. Sometimes, individuals are hired based on nepotism and without proper education in the fields. It becomes a bigger problem, when the directors hiring them are also bad fits for their positions. In the healthcare sector, it means lives are at stake, and it has severe consequences. Not only jeopardizing patients’ lives, but also compromising data reliability. A consultant shared an alarming example: in one instance a hospital reported a suspiciously high number of cholera cases, but when authorities tested patients the results were negative. While he didn’t solely attribute this to opportunism, he emphasized the widespread issue of misdiagnosis. In many cases doctors, nurses or health workers report cases based on symptoms alone without lab confirmation. This not only distorts the true picture of the outbreak but also leads to inappropriate treatment further contributing to antimicrobial resistance such as MDR-TB. In addition, educated lab workers are pressured to take on more responsibility than they can handle – this is mismanagement. Thus, the specialists become generalists and won’t have proper time to analyze the results.
We need to fix this issue by hiring more qualified laboratory technicians and directors. All workers must be presenting relevant education papers documenting their skills for laboratory work. Furthermore, they must receive training from competent supervisors.
Bad quality medications are a huge problem in Somalia
Another major issue is the unregulated pharmacy sector. Somalia’s pharmaceutical industry has been in crisis since the civil war, leaving the country flooded with unregulated and often counterfeit medicines. Many pharmacies operate without proper quality checks, exposing patients to expired or falsified drugs. Weak healthcare infrastructure and lack of enforcement allow importers to use Somalia as a dumping ground for unsafe medications. This poses severe health risks, with some experts comparing counterfeit drugs to weapons due to their deadly impact. Strengthening regulation and healthcare policies is crucial (Fight the fakes). There is also a push back from industry insiders. With an open market and fierce competition pharmacies often stock drugs that are the most profitable rather than those that are most needed. In addition, storage of medication can also be problematic, due to the rising cost of electricity (Puntland post). Currently, the government is joining the world in the fight against fake medicines by introducing new regulations in line with African Union and WHO standards.
Finally, the lack of coordination and system integration between different Somali health agencies weakens data collection, outbreak response, and communication efficiency. This is worsened by inconsistent reporting systems.
Concluding remarks and looking forward
Somalia has come a long way in fighting infectious diseases, but to achieve meaningful progress much more needs to be done. Gradual improvements in the health sector are required but without proper funding, regulation, and coordination progress remains slow. Addressing these challenges is essential to combating these deadly diseases.
This article has provided an in-depth overview on the health challenges of Somali people. It introduced both the steps taken from the government and domestic problems that hinder the process. By exploring more than one angle we aimed to give you the reader a comprehensive understanding of this crisis.
Throughout the process of writing the article we approached the topic with curiosity asking two fundamental questions: what is happening and why is it happening? Motivated by the thousands of preventable deaths, we sought answers, but now we turn the question back to you, the reader, what role do you play in this situation? How can you help?
We will give you some clues so you won’t be left in the dark. Most of you readers are diaspora Somalis, and Somalia needs your skills to develop further. Somalia needs better management and more skilled medical personnel and above all long-term internal funding. Although money won’t solve all these issues, most of the issues we have covered are funding related. However for surveillance methods to get the optimal result it has to be accompanied by increased lab capacity and enhanced pathogen detection. Personally, we plan on continuing the work by focusing on the latter – implementing better laboratory detection tools to optimize surveillance of infectious diseases in Somalia.


Mashallah it’s good to know we have critical thinkers that could discuss these issues and find solutions 🫡❤️
Really insightful read. It’s so important to keep spreading awareness about infectious diseases; this kind of work makes a difference.